
Clinico-radiological predictors of positive rigid bronchoscopy findings in children with suspected tracheobronchial foreign body aspiration
Introduction
Tracheobronchial foreign body aspiration (TFBA) is a common paediatric emergency department presentation due to a tendency of infants and young children to place a range of objects in their mouths, as well as the paediatric airway anatomy (1,2). It can result in significant morbidity and mortality for children less than 3 years of age (3-6), including pneumonia, lung abscesses or bronchiectasis. A prompt and accurate diagnosis is therefore important in the management of this condition.
Children with suspected TFBA have variable clinical presentations, with symptoms such as cough, wheeze, noisy breathing or respiratory distress (7-10). Few children present with an actual witnessed episode of foreign body (FB) aspiration. Furthermore, physical examination findings and radiological investigations such as plain chest radiography (CXR) often do not provide additional diagnostic information (7,9,11,12).
Given the difficulty of accurately diagnosing children with suspected TFBA clinically, rigid bronchoscopy (RB) examination remains both the definitive diagnostic approach as well as a treatment modality if required (2,13). However, this procedure is associated with significant risks such as airway trauma and pneumothorax, along with perioperative complications and potential long-term effects associated with general anaesthetic in children (6,14,15). Previously reported rates of negative RB findings greatly vary, ranging from 10 to 75% (2,3,12,16,17).
This is the first study to assess the diagnostic accuracy of various clinical and radiological findings in predicting the identification of TFBA at RB in the Australian paediatric population. Our aim was to identify clinical and radiological findings that could potentially identify children who were unlikely to have positive TFBA identification at RB to potentially reduce the rate of negative RB examination.
Methods
This was a single health service retrospective study of consecutive paediatric patients presenting with suspected lower respiratory tract FB from November 2010 to May 2016. Ethical approval was obtained from the Monash Health Human Research Ethics Low Risk Review Panel.
Inclusion criteria included paediatric patients 16 years or younger presenting with suspected TFBA who underwent RB as part of their management. All procedures were performed using RB with an optical telescope and high definition camera. Occasionally, flexible bronchoscopy was also performed to further exclude distal bronchial tree FB.
Information collected included age, gender, delay in presentation after suspected TFBA and date of hospital presentation. Symptoms of aspiration recorded included witnessed acute choking or coughing episodes, wheezing or clinical examination findings of reduced air entry or abnormal breath sounds, as well as CXR findings of suspected FB, collapse, consolidation or hyperinflation. Operative findings were also recorded. Surgical and anaesthetic complications were noted.
Blinded evaluation of preoperative clinical data (desaturation, wheeze, reduced air entry) and preoperative CXR were used to test diagnostic performance of individual and combined predictors of TFBA. Categorical data are presented in percentages while continuous data are presented as mean and median. The diagnostic accuracy [sensitivity, specificity, positive and negative predictive value (NPV)] of patient history, examination findings and radiological investigations was compared with the reference standard of bronchoscopic examination. Differences between positive and negative RB findings with regards to various factors were determined with Fisher’s exact test. A P value of less than 0.05 was deemed statistically significant.
Results
Seventy-six children presented to Monash Health between November 2010 and May 2016, of which 43 met criteria for analysis. Patients were excluded if medical records or imaging results were not available (n=1), if the FB was located at or above the level of the glottis (n=3), if CXR images were not available (n=27), or if CXR showed inadequate inspiration (n=2). There were 27 males (63%) and 16 females (37%) (Table 1).
Table 1
| Patient factor | N | Percentage % |
|---|---|---|
| Age | ||
| 0–3 years | 31 | 72.1 |
| >3 years | 12 | 27.9 |
| Median | 25 months | – |
| Gender | ||
| Male | 27 | 63.0 |
| Female | 16 | 37.0 |
| Comorbidities | ||
| Asthma | 3 | 7.0 |
The median age was 25 months with 31 patients (72.1%) being less than 3 years of age. Median day of presentation after suspected inhalation was 0 days. Three patients had a history of diagnosed asthma.
Organic FBs were the most common (55.9% of all FBs), with the majority being nuts or pieces of vegetable (Table 2). Inorganic FBs represented 44.1% of all FBs, with the majority being pins. Only 7 FBs were radiopaque (20.6%). No FBs were identified in 9 children (20.9%) who underwent RB. Foreign bodies were most commonly found in the right main bronchus (32.3%) (Table 3).
Table 2
| Foreign body type | N | Percentage % |
|---|---|---|
| No foreign body | 9 | 20.9 |
| Organic foreign body | 19 | 44.2 |
| Nuts | 8 | 18.6 |
| Seeds | 3 | 7.0 |
| Carrots | 2 | 4.7 |
| Other organic material | 6 | 14.0 |
| Inorganic foreign body | 15 | 34.9 |
| Pins (radio-opaque) | 6 | 14.0 |
| Stone (radio-opaque) | 1 | 2.3 |
| Plastic | 6 | 14.0 |
| Other inorganic material | 2 | 4.7 |
Table 3
| Anatomical location | N | Percentage |
|---|---|---|
| Trachea | 8 | 18.6 |
| Left main bronchus | 11 | 25.6 |
| Right main bronchus | 14 | 32.6 |
| Left intermediate bronchus | 1 | 2.3 |
There was no significant difference between the number of children with and without FB found on RB with regards to age (P=0.405), gender (P=0.706) and day of presentation after suspected inhalation (P=0.696) (Table 4).
Table 4
| Patient factor | Likelihood of foreign body found at RB | Fisher’s exact test (P value) |
|---|---|---|
| Age | 0.405 | |
| 0–3 years | 23/31 (74.2%) | |
| >3 years | 11/12 (91.7%) | |
| Gender | 0.706 | |
| Male | 22/27 (81.5%) | |
| Female | 12/16 (75.0%) | |
| Day of presentation | 0.696 | |
| Day of suspected inhalation | 23/28 (82.1%) | |
| After day of suspected inhalation | 11/15 (73.3%) | |
| Clinical symptoms | 0.407 | |
| Coughing/choking episode | 24/32 (75.0%) | |
| Others | 10/11 (90.9%) | |
| Auscultation | 0.294 | |
| Positive findings | 26/29 (90.0%) | |
| Negative findings | 8/14 (57.1%) | |
| Chest X-ray | 1.000 | |
| Positive findings | 24/30 (80.0%) | |
| Negative findings | 10/13 (76.9%) | 0.405 |
Thirty-two children (74.4%) presented with a primary symptom of an acute onset coughing or choking episode, while 11 presented with other symptoms such as wheezing (Table 4). Neither of these symptoms was positively associated with the presence of a FB at RB (P=0.407).
Sixty-seven point four percent of children had abnormal chest auscultation findings of unilateral abnormal or reduced breath sounds. There was no significant difference between children with and without FB found on RB with regards to normal or non-diagnostic auscultation findings (P=0.294). The side of positive auscultation findings correlated 57.1% of the time with the side of TFBA finding on RB.
Moreover, no significant difference was found between those who had normal and abnormal CXR findings of suspected FB (P=0.6566), collapse (P=1.0000), consolidation (P=0.0948), hyperinflation (P=0.1710), or any abnormal CXR finding (P=1.000).
Thirty-five percent of children had an inspiratory and expiratory radiograph, and 16% had a lateral as well as an anteroposterior (AP) view. The positive predictive value (PPV) of auscultation findings was 0.90 with a 95% confidence interval of 0.77–0.96, which approached but did not reach statistical significance when compared with clinical and CXR findings (Table 5). No significant difference was found in specificity or negative predictive values (NPV) between clinical findings, chest auscultation and CXR findings, with a large 95% confidence interval for the sensitivity of each of the three predictive factors (Table 5). Hyperinflation (sensitivity 24%, specificity 100%) on CXR was found to be more specific than collapse or consolidation (sensitivity 26%, specificity 44%) for predicting the presence of a FB.
Table 5
| Clinico-radiological factor | Sensitivity (95% CI) | Specificity (95% CI) | PPV (95% CI) | NPV (95% CI) |
|---|---|---|---|---|
| Clinical symptoms | 0.71 (0.53–0.85) | 0.11 (0.003–0.48) | 0.75 (0.69–0.80) | 0.09 (0.01–0.41) |
| Coughing/choking episode | 0.03 (0.01–0.15) | 1.00 (0.66–1.00) | 1.00 (0.64–1.00) | 0.21 (0.20–0.22) |
| Wheezing | 0.26 (0.13–0.44) | 0.89 (0.52–1.00) | 0.90 (0.57–0.98) | 0.24 (0.19–0.30) |
| Auscultation | 0.76 (0.59–0.89) | 0.67 (0.30–0.93) | 0.90 (0.77–0.96) | 0.43 (0.26–0.64) |
| CXR | 0.71 (0.53–0.85) | 0.33 (0.07–0.70) | 0.80 (0.71–0.87) | 0.23 (0.09–0.46) |
| Suspected FB | 0.24 (0.11–0.41) | 0.89 (0.52–1.00) | 0.89 (0.53–0.98) | 0.24 (0.19–0.29) |
| Collapse | 0.18 (0.07–0.35) | 0.78 (0.40–0.97) | 0.75 (0.42–0.93) | 0.20 (0.15–0.27) |
| Consolidation | 0.09 (0.02–0.24) | 0.67 (0.30–0.93) | 0.50 (0.19–0.81) | 0.16 (0.11–0.24) |
| Hyperinflation | 0.24 (0.11–0.41) | 1.00 (0.66–1.00) | 1.00 (0.64–1.00) | 0.26 (0.22–0.29) |
PPV, positive predictive value; NPV, negative predictive value; CXR, chest radiography; FB, foreign body.
Of the 14 children with normal or non-diagnostic chest auscultation findings, 6 (42.9%) had normal lower airways on subsequent RB. The combination of an abnormal CXR and/or any clinical abnormality allowed better prediction of a FB (sensitivity 0.91 and specificity 0.22) but still a relatively high false positive rate (14.0%).
There were 2 complications (4.7%). One child developed a postoperative lower respiratory tract infection which resolved with antibiotics, whilst another had a mucosal injury to the pyriform fossa which was managed conservatively. Unfortunately, one child was brought to hospital in cardiac arrest and, despite successful removal of the FB, died as a result of hypoxic brain injury.
Discussion
The prompt and accurate diagnosis of TFBA in children is important to prevent mortality or significant morbidity, including pneumonia, lung abscesses and bronchiectasis (3-6). However, if clinical and radiological findings are non-diagnostic, children with suspected TFBA often require RB examination (18,19).
Similar to previous studies, our data showed the majority of children presenting with TFBA to be less than three years of age (9,13,17). Moreover, the majority of FBs aspirated were food material (9,11). These may be explained by the developing neuromusculature and the lack of a complete set of molars for the coordination of pharyngeal swallow, respiratory, and oesophageal functions in children in failing to adequately protect their airways from foreign bodies (1,20), the calibre of the tracheobronchial anatomy in relation to the size of foreign bodies, and also the exploratory nature of children in this age group, particularly with placing objects into their mouths (13,17).
TFBA were most commonly located in the right main bronchus, consistent with the published literature, due to its more acute angle and wider calibre in relation to the rest of the tracheobronchial anatomy (11,21). This study demonstrated positive RB findings in 79.1%. The reported rates in the literature greatly vary, ranging from as low as 25% up to 90% (2,3,12,16,17). This may be due to the variable indications and referral processes for RB examinations in different paediatric hospitals.
Commonly reported clinical symptoms associated with TFBA are acute episodes of choking, coughing or wheezing, along with auscultation findings of unilateral abnormal or reduced breath sounds (3,19,22-24). These symptoms and clinical findings have often been shown to be the most sensitive and specific in the diagnosis of suspected TFBA (9,12,16). Although a large proportion of children (77.8%) in this study presented with symptoms of choking, cough or wheeze, there was no significant difference in the rates of positive RB findings between children with and without these symptoms. This may be due to the relatively small cohort in this study as well as the difficulty in establishing an accurate history retrospectively. The PPV of positive auscultation findings was higher than that of clinical and CXR findings but failed to reach statistical significance.
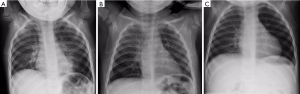
CXR findings associated with TFBA include unilateral hyperinflation, collapse or consolidation (7,11,12) (Figure 1). However, this study showed inconsistent radiographic technique in assessing TFBA with satisfactory inspiratory and expiratory films and did not identify significantly greater sensitivity of CXR findings compared to auscultation findings. This is consistent with data from the literature in which the majority of aspirated FBs are radiolucent (79.4% in this study), and most children present on the day of suspected aspiration when there are often no CXR findings of diagnostic value, with the first radiological findings being hyperinflation, which is reflected by its higher specificity in this study (3,9,19,25). Moreover, this study only found a small proportion of radio-opaque FBs (20.6%), which is similar to previously reported values (9,11,17).
Limitations of this study include relatively small sample size, which may have resulted in a type II error in attempting to identify predictors of positive RB in the setting of suspected TBFA. Similar studies had shown conflicting results, with Heyer et al. concluding that witnessed aspiration, hyperinflation on CXR and white cell count to be statistically significant predictors of positive RB (12) while Divarci et al. had found that all positive clinical, examination and radiological findings were statistically significant predictors (26). Therefore, larger studies may be required to further assess clinico-radiological predictors of positive RB. The retrospective nature of our study also meant that radiographic technique was inconsistent between subjects with only an AP inspiratory view being consistently performed, and expiratory and lateral views in a minority of patients. This may have reduced the measured sensitivity and specificity of CXR. Finally, it was unclear what exact information the managing otolaryngologist used to decide how patients were selected for RB. Therefore, selection bias could not be excluded in our cohort due to patients who did not proceed to RB being excluded a priori from this study.
RB examination remains the gold standard for the definitive diagnosis and management of TFBA (2,13). RB is associated with rare but serious complications, including upper and lower airway trauma, laryngospasm, bronchospasm and pneumothorax (27-29). Hasdiraz et al. reports a rate of 4% for chest infections, 0.6% for airway trauma and 0.2% for pneumothorax out of 1,035 RB’s performed (28). A recent review by Stahl et al. reported complication rates from RB ranging from less than 0.1 to 13% (14). Although general anaesthesia for RB is associated with low morbidity, significant adverse events such as pneumonia, respiratory failure or cardiovascular compromise can occur in the perioperative period (6,15). Moreover, there are conflicting results from recent studies regarding the possible long-term effects of general anaesthesia in early childhood, with some studies finding long-term effects such as neurocognitive impairment as well as behavioural and emotional consequences (30-32), while others finding no significant long-term effects (33).
In this study, 20.9% of children with clinically suspected TFBA had normal (negative) RB examinations. This is in keeping with the current literature, with negative bronchoscopy reported in 25% to 90% of cases (2,3,12,16,17). Although this study has shown a relatively high PPV for clinical, auscultation and CXR findings, this is often a difficult group to diagnose, and it is therefore important to balance the risks of RB and general anaesthetic with those associated with a missed diagnosis of FB aspiration in this subset of children with suspected TFBA.
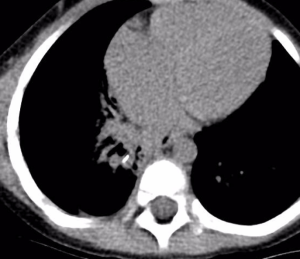
Low dose multidetector computed tomography (MDCT) may be utilised as an alternative diagnostic tool for children with an unclear history of suspected TFBA without positive clinical or radiological findings; with studies showing this to be sensitive and specific in detecting aspirated FBs and hence reduce the likelihood of an unnecessary general anaesthetic and negative RB examination (34-37). Figure 2 shows an example of a right sided segmental bronchiole FB found on MDCT. If the MDCT is suggestive of a FB then RB would be indicated, but if the MDCT is negative, the procedure might be avoidable in a normoxaemic child. Moreover, although traditional CT in children had been associated with breast, thyroid and haematological malignancy (38-40), use of child-sized lower kVp techniques and recent advances in ultra-low dose MDCT incorporating iterative reconstruction have significantly reduced radiation dosage for these investigations to as little as 1.5 mGy or less for chest CT (41), with conventional CXR, depending on the number of projections, delivering up to 0.9 mGy (42). Further prospective studies may be useful in assessing these investigations including technical challenges in obtaining technically adequate low-dose unsedated CT in young children, potential for overdiagnosis of airway abnormalities that do not represent FB, and logistical issues with performing and interpreting low dose paediatric CT studies after normal working hours (43).
Conclusions
TFBA is associated with potentially significant morbidity and mortality in children, therefore prompt and accurate diagnosis is often required. Children with non-specific history of aspiration and non-diagnostic clinical or radiological findings may undergo a negative RB examination under general anaesthetic. RB, even when negative, is costly and not without rare but serious risks, both in the perioperative period and longer term. It would therefore be beneficial to avoid unnecessary (negative) bronchoscopies. Newer techniques such as ultra-low dose MDCT may be useful in the management of these children, and prospective clinical trials, evaluating the clinical efficacy and cost of incorporation of low dose CT at defined points in the diagnostic algorithm, are warranted.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/ajo.2018.01.07). PP serves as an unpaid editorial board member of Australian Journal of Otolaryngology. JR serves as an unpaid editorial board member of Australian Journal of Otolaryngology. The other authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). Ethical approval was obtained from the Monash Health Human Research Ethics Low Risk Review Panel. Informed consent was waived due to the retrospective nature of the study.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Higo R, Matsumoto Y, Ichimura K, et al. Foreign bodies in the aerodigestive tract in pediatric patients. Auris Nasus Larynx 2003;30:397-401. [Crossref] [PubMed]
- Black RE, Johnson DG, Matlak ME. Bronchoscopic removal of aspirated foreign bodies in children. J Pediatr Surg 1994;29:682-4. [Crossref] [PubMed]
- Sersar SI, Rizk WH, Bilal M, et al. Inhaled foreign bodies: presentation, management and value of history and plain chest radiography in delayed presentation. Otolaryngol Head Neck Surg 2006;134:92-9. [Crossref] [PubMed]
- Reilly J, Thompson J, MacArthur C, et al. Pediatric aerodigestive foreign body injuries are complications related to timeliness of diagnosis. Laryngoscope 1997;107:17-20. [Crossref] [PubMed]
- Mu L, He P, Sun D. The causes and complications of late diagnosis of foreign body aspiration in children. Report of 210 cases. Arch Otolaryngol Head Neck Surg 1991;117:876-9. [Crossref] [PubMed]
- Fidkowski CW, Zheng H, Firth PG. The anesthetic considerations of tracheobronchial foreign bodies in children: a literature review of 12,979 cases. Anesth Analg 2010;111:1016-25. [PubMed]
- Bittencourt PF, Camargos PA, Scheinmann P, et al. Foreign body aspiration: clinical, radiological findings and factors associated with its late removal. Int J Pediatr Otorhinolaryngol 2006;70:879-84. [Crossref] [PubMed]
- Hui H, Na L, Zhijun C, et al. Therapeutic experience from 1428 patients with pediatric tracheobronchial foreign body. J Pediatr Surg 2008;43:718-21. [Crossref] [PubMed]
- Orji FT, Akpeh JO. Tracheobronchial foreign body aspiration in children: how reliable are clinical and radiological signs in the diagnosis? Clin Otolaryngol 2010;35:479-85. [Crossref] [PubMed]
- Tang FL, Chen MZ, Du ZL, et al. Fibrobronchoscopic treatment of foreign body aspiration in children: an experience of 5 years in Hangzhou City, China. J Pediatr Surg 2006;41:e1-5. [Crossref] [PubMed]
- Boufersaoui A, Smati L, Benhalla KN, et al. Foreign body aspiration in children: experience from 2624 patients. Int J Pediatr Otorhinolaryngol 2013;77:1683-8. [Crossref] [PubMed]
- Heyer CM, Bollmeier ME, Rossler L, et al. Evaluation of clinical, radiologic, and laboratory prebronchoscopy findings in children with suspected foreign body aspiration. J Pediatr Surg 2006;41:1882-8. [Crossref] [PubMed]
- Shields TW, LoCicero J 3rd, Reed CE, et al. General thoracic surgery. 7th ed. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins, 2009.
- Stahl DL, Richard KM, Papadimos TJ. Complications of bronchoscopy: A concise synopsis. Int J Crit Illn Inj Sci 2015;5:189-95. [Crossref] [PubMed]
- Tomaske M, Gerber AC, Weiss M. Anesthesia and periinterventional morbidity of rigid bronchoscopy for tracheobronchial foreign body diagnosis and removal. Paediatr Anaesth 2006;16:123-9. [Crossref] [PubMed]
- Emir H, Tekant G, Beşik C, et al. Bronchoscopic removal of tracheobroncheal foreign bodies: value of patient history and timing. Pediatr Surg Int 2001;17:85-7. [Crossref] [PubMed]
- Oncel M, Sunam GS, Ceran S. Tracheobronchial aspiration of foreign bodies and rigid bronchoscopy in children. Pediatr Int 2012;54:532-5. [Crossref] [PubMed]
- Dunn GR, Wardrop P, Lo S, et al. Management of suspected foreign body aspiration in children. Clin Otolaryngol Allied Sci 2004;29:286. [Crossref] [PubMed]
- Tokar B, Ozkan R, Ilhan H. Tracheobronchial foreign bodies in children: importance of accurate history and plain chest radiography in delayed presentation. Clin Radiol 2004;59:609-15. [Crossref] [PubMed]
- Lau C. Development of Suck and Swallow Mechanisms in Infants. Ann Nutr Metab 2015;66:7-14. [Crossref] [PubMed]
- Fennira H, Ben Slimene D, Bourguiba M, et al. Tracheobronchial foreign bodies. Diagnostic and therapeutic aspects in children. Tunis Med 2004;82:817-26. [PubMed]
- Pinzoni F, Boniotti C, Molinaro SM, et al. Inhaled foreign bodies in pediatric patients: review of personal experience. Int J Pediatr Otorhinolaryngol 2007;71:1897-903. [Crossref] [PubMed]
- Rizk H, Rassi S. Foreign body inhalation in the pediatric population: lessons learned from 106 cases. Eur Ann Otorhinolaryngol Head Neck Dis 2011;128:169-74. [Crossref] [PubMed]
- Roda J, Nobre S, Pires J, et al. Foreign bodies in the airway: a quarter of a century's experience. Rev Port Pneumol 2008;14:787-802. [Crossref] [PubMed]
- Svedström E, Puhakka H, Kero P. How accurate is chest radiography in the diagnosis of tracheobronchial foreign bodies in children? Pediatr Radiol 1989;19:520-2. [Crossref] [PubMed]
- Divarci E, Toker B, Dokumcu Z, et al. The multivariate analysis of indications of rigid bronchoscopy in suspected foreign body aspiration. Int J Pediatr Otorhinolaryngol 2017;100:232-7. [Crossref] [PubMed]
- Facciolongo N, Patelli M, Gasparini S, et al. Incidence of complications in bronchoscopy. Multicentre prospective study of 20,986 bronchoscopies. Monaldi Arch Chest Dis 2009;71:8-14. [PubMed]
- Hasdiraz L, Oguzkaya F, Bilgin M, et al. Complications of bronchoscopy for foreign body removal: experience in 1,035 cases. Ann Saudi Med 2006;26:283-7. [Crossref] [PubMed]
- Petrella F, Borri A, Casiraghi M, et al. Operative rigid bronchoscopy: indications, basic techniques and results. Multimed Man Cardiothorac Surg 2014;2014. pii: mmu006.
- Backeljauw B, Holland SK, Altaye M, et al. Cognition and Brain Structure Following Early Childhood Surgery With Anesthesia. Pediatrics 2015;136:e1-12. [Crossref] [PubMed]
- Bakri MH, Ismail EA, Ali MS, et al. Behavioral and emotional effects of repeated general anesthesia in young children. Saudi J Anaesth 2015;9:161-6. [Crossref] [PubMed]
- Sun L. Early childhood general anaesthesia exposure and neurocognitive development. Br J Anaesth 2010;105:i61-8. [Crossref] [PubMed]
- Sun LS, Li G, Miller TL, et al. Association Between a Single General Anesthesia Exposure Before Age 36 Months and Neurocognitive Outcomes in Later Childhood. JAMA 2016;315:2312-20. [Crossref] [PubMed]
- Bai W, Zhou X, Gao X, et al. Value of chest CT in the diagnosis and management of tracheobronchial foreign bodies. Pediatr Int 2011;53:515-8. [Crossref] [PubMed]
- Jung SY, Pae SY, Chung SM, et al. Three-dimensional CT with virtual bronchoscopy: a useful modality for bronchial foreign bodies in pediatric patients. Eur Arch Otorhinolaryngol 2012;269:223-8. [Crossref] [PubMed]
- Koşucu P, Ahmetoğlu A, Koramaz I, et al. Low-dose MDCT and virtual bronchoscopy in pediatric patients with foreign body aspiration. AJR Am J Roentgenol 2004;183:1771-7. [Crossref] [PubMed]
- Yang C, Hua R, Xu K, et al. The role of 3D computed tomography (CT) imaging in the diagnosis of foreign body aspiration in children. Eur Rev Med Pharmacol Sci 2015;19:265-73. [PubMed]
- Krille L, Dreger S, Schindel R, et al. Risk of cancer incidence before the age of 15 years after exposure to ionising radiation from computed tomography: results from a German cohort study. Radiat Environ Biophys 2015;54:1-12. [Crossref] [PubMed]
- Mathews JD, Forsythe AV, Brady Z, et al. Cancer risk in 680,000 people exposed to computed tomography scans in childhood or adolescence: data linkage study of 11 million Australians. BMJ 2013;346:f2360. [Crossref] [PubMed]
- Pearce MS, Salotti JA, Little MP, et al. Radiation exposure from CT scans in childhood and subsequent risk of leukaemia and brain tumours: a retrospective cohort study. Lancet 2012;380:499-505. [Crossref] [PubMed]
- Lee JY, Chung MJ, Yi CA, et al. Ultra-low-dose MDCT of the chest: influence on automated lung nodule detection. Korean J Radiol 2008;9:95-101. [Crossref] [PubMed]
- Babikir E, Hasan HA, Abdelrazig A, et al. Radiation dose levels for conventional chest and abdominal X-ray procedures in elected hospitals in Sudan. Radiat Prot Dosimetry 2015;165:102-6. [Crossref] [PubMed]
- Kim Y, Kim YK, Lee BE, et al. Ultra-Low-Dose CT of the Thorax Using Iterative Reconstruction: Evaluation of Image Quality and Radiation Dose Reduction. AJR Am J Roentgenol 2015;204:1197-202. [Crossref] [PubMed]
Cite this article as: Kwok MM, Wong A, Paddle P, Goergen S, Rimmer J. Clinico-radiological predictors of positive rigid bronchoscopy findings in children with suspected tracheobronchial foreign body aspiration. Aust J Otolaryngol 2018;1:11.


