
Otitis media and quality of life in NSW Aboriginal children
Introduction
Chronic ear disease affects Aboriginal children at higher rates than their non-Aboriginal counterparts (1). The long-term adverse effects, aside from complications, are known in relation to education, development and employment (2). There are also significant short-term effects on QoL with recurrent acute illness (3). Little data has been published on the quality of life (QoL) of children living with ear disease in Australia. We investigated the utility of the Otitis Media-6 (OM-6) questionnaire (3) among Aboriginal and non-Aboriginal parents/caregivers to assess the QoL experienced by children undergoing surgery for ventilation tube (VT, grommet) insertion to treat recurrent otitis media (OM) and otitis media with effusion (OME).
The OM-6 questionnaire is a tool developed in the United States specifically for assessment of the impact of recurrent acute OM and OME (4). The OM-6 requires parents/caregivers to rate their child’s QoL on a scale of 1–7 for the following six domains: physical suffering, hearing loss, speech impairment, emotional distress, activity limitations and caregiver concerns. It was chosen for this study because of its ease of use and established acceptability for assessing QoL in OM (5,6). The OM-6 was used previously to assess QoL of 53 South Australian children who received VTs for recurrent acute OM and OME (7). The study by Chow et al. was valuable in demonstrating QoL improvement across the six questionnaire domains following VT surgery, but it did not provide information specifically relating to Aboriginal identification. Our primary aim was to establish the suitability of the OM-6 for QoL studies of ear disease among Aboriginal Australians accessing surgical intervention in urban, regional and rural areas of the Hunter New England Local Health District (HNELHD) of NSW.
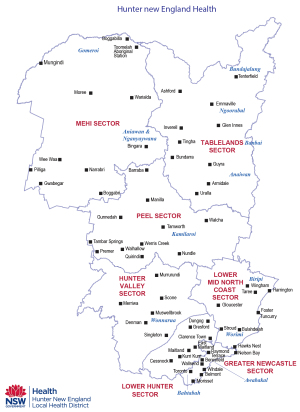
Within the Aboriginal population there is diversity of culture, lifestyles and geographical locations. The HNELHD provides health services to around 920,370 people, of whom approximately 5% (52,990) identify as Aboriginal (8). The base for tertiary level health services is the metropolitan coastal city of Newcastle, 200 km north of Sydney. The HNELHD extends north and west across 25 local government areas to include both large and small regional, rural and remote centres and covers many Aboriginal nations; Worimi to the east, Gomeroi to the west, Bundjalung to the north and Awabakal to the south, including many different groups within (8) (Figure 1). Due to the centralisation of Ear, Nose and Throat (ENT) services in the metropolitan hub, regional access to specialist pathways including operative intervention can be difficult. The problem is compounded by long travel distances across the HNELHD to access specialised clinics for the diagnosis and treatment of OM. This article is presented in accordance with the STROBE checklist (available at https://ajo.amegroups.com/article/view/10.21037/ajo-21-24/rc).
Methods
Ethical considerations
The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). Ethics approval for the Quality of Life project was obtained from the Hunter New England Human Research Ethics Committee (ref: 2020/ETH00170). The use of data collected using the OM-6 survey tool among HNELHD Aboriginal research participants was approved by the Aboriginal Health and Medical Research Council Ethics Committee (1703/20). Informed consent for participation in the OM-6 study was obtained by the research co-ordinator from all parents/caregivers prior to their child’s surgery and it was explained that all medical procedures were independent of the research study.
Participant recruitment
Aboriginal and non-Aboriginal parents/carers were recruited to the study opportunistically, without reference to their Aboriginality or otherwise. Recruitment took place in the paediatric wards at two HNELHD public hospitals on the morning of their child’s VT surgery. The project extended over 20 months from February 2018 to September 2019 and involved 37 individual surgical lists on separate dates. Parents/carers of children undergoing VT surgery were invited to complete the study questionnaires. Children were not selected out of the study on the basis of their other health status or additional surgical procedures, such as tonsillectomy or adenoidectomy, as the project was a pilot study focused primarily on parent/carer engagement with the OM-6 questionnaire, not an assessment of the health effects of the medical intervention.
QoL survey
On the morning of surgery, following informed consent, parents/carers were asked to self-administer the OM-6 questionnaire (paper copy) together with a brief demographic questionnaire. The OM-6 was administered a second time by phone conversation between the research co-ordinator and the parent/carer at a median 6 weeks (interquartile range of 5–7 weeks) after the day of surgery.
The OM-6 comprises of 6 questions measuring different aspects of OM-related QOL: responses for Q1–4 (physical suffering, hearing loss, speech impairment, and emotional distress) are scored 1 (not present/no problem) to 7 (extreme problem), Q5 (activity limitations) is scored as 1 (not limited at all) to 7 (severely limited), and Q6 (caregiver concerns) is scored 1 (none of the time) to 7 (all of the time). Change scores between pre- and post-surgery were calculated. The difference in measures was interpreted as an indicator of parental/caregiver perceptions of the impact that ear disease imposed on the child’s QoL before and after surgery. An overall score was created as the average of the 6 individual domains. A reduction in the score for each question represents a perceived improvement in OM-related QoL.
Statistical analysis
Data were stored in a REDCap (Vanderbuilt University) database hosted at the Hunter Medical Research Institute in Newcastle (Awabakal). All statistical analyses were conducted using SAS v9.4 (SAS Institute, Cary, North Carolina, USA); P<0.05 (two-tailed) was used to indicate statistical significance.
Descriptive statistics of patient characteristics and QoL measures (baseline and follow-up) were produced overall, and by Aboriginal identification. Means (SD) and medians (Q1, Q3) were calculated for continuous data; frequencies and proportions (%) were reported for categorical variables. Corresponding P values for differences in study variables between Aboriginal and non-Aboriginal participants were generated using Chi-squared tests for categorical variables while independent sample t-tests and Wilcoxon signed-rank tests were used for continuous measures. Association between antibiotic use in the last month and number of infections in the past year was investigated by Fisher’s exact test.
Linear mixed models enabled analyses on repeated measures to be performed while retaining data on participants with missing observations. These models were used to assess change in QoL for individual domains as well as overall scores before and after surgery (n=101). A random intercept was employed to account for correlations of pre and post outcome measures within patients in the univariable models of time. Differences in least squares (LS) means estimates and 95% confidence intervals (CIs) were determined with relevant P values. Intraclass correlation coefficients (ICCs) for each mixed model were provided to describe the correlation of QoL within a participant over time.
Linear mixed models were also used to compare change in QoL by Aboriginal identification/non-identification. Modelling included time, Aboriginal identification and a two-way interaction term to assess change in trends over time as well as a random intercept. LS means estimates (95% CI) were produced for each time point by Aboriginal identification. Differences in estimates were calculated to assess both time and Aboriginal effects; P values of the overall interaction effect in each model were also provided from Type III testing.
Results
All parents/caregivers of Aboriginal and non-Aboriginal children invited to participate on the day of their child’s VT surgery agreed to complete the questionnaires. In total, 101 OM-6 and demographic questionnaires were completed, with the vast majority of parents not requesting any assistance to complete the forms. Parents were instructed to focus on ear problems alone, as co-morbidities were not included for assessment.
Of the 101 children, 53% identified as Aboriginal, while 46% identified as non-Aboriginal Australian, with other ethnicities being rare (1%). These figures affirmed an anticipated higher proportion of Aboriginal children requiring specialist ENT treatments for chronic ear disease in the HNELHD regions. Of the total cohort, 67% of VT patients were male, while 33% were female.
The results, summarised in Table 1, show that there were no significant differences between Aboriginal and non-Aboriginal children for living at a rural address, median age at surgery (6 years), infection patterns, antibiotic use in the past month and demographic characteristics of the household in which a child lived.
Table 1
| Characteristics | Class/statistic | Aboriginal identification | Total (N=101) | P value | |
|---|---|---|---|---|---|
| No (n=47) | Yes (n=54) | ||||
| Gender | Male | 32 (68%) | 36 (67%) | 68 (67%) | 0.8795 |
| Female | 15 (32%) | 18 (33%) | 33 (33%) | ||
| Rurality | Major city | 32 (70%) | 30 (58%) | 62 (63%) | 0.2336 |
| Inner regional | 13 (28%) | 17 (33%) | 30 (31%) | ||
| Outer regional | 1 (2.2%) | 5 (9.6%) | 6 (6.1%) | ||
| Age of first infection | Young baby (0–6 months) | 24 (51%) | 27 (52%) | 51 (52%) | 0.9289 |
| Older baby (6–12 months) | 21 (45%) | 22 (42%) | 43 (43%) | ||
| N/A | 2 (4.3%) | 3 (5.8%) | 5 (5.1%) | ||
| Infections in past year | 1, 2 or 3 | 22 (51%) | 23 (48%) | 45 (49%) | 0.8785 |
| 4, 5 or 6 | 8 (19%) | 11 (23%) | 19 (21%) | ||
| More than 6 | 13 (30%) | 14 (29%) | 27 (30%) | ||
| Antibiotics in past month | No | 34 (76%) | 38 (79%) | 72 (77%) | 0.6772 |
| Yes | 11 (24%) | 10 (21%) | 21 (23%) | ||
| Age at surgery | Mean (SD) | 5.66 (2.84) | 6.04 (2.43) | 5.86 (2.62) | 0.4735 |
| Median (Q1, Q3) | 6 (3, 8) | 6 (4, 7) | 6 (4, 7) | 0.5310 | |
| Weeks between surveys | Mean (SD) | 5.70 (1.42) | 6.03 (1.19) | 5.86 (1.31) | |
| Median (Q1, Q3) | 6 (5, 6) | 6 (5, 7) | 6 (5, 7) | 0.2754 | |
| Children in house | Mean (SD) | 2.15 (1.14) | 2.15 (1.10) | 2.15 (1.11) | |
| Median (Q1, Q3) | 2 (1, 3) | 2 (2, 3) | 2 (1, 3) | 0.6882 | |
| Other children with ear infection | Mean (SD) | 0.53 (0.69) | 0.89 (0.93) | 0.72 (0.84) | |
| Median (Q1, Q3) | 0 (0, 1) | 1 (0, 1) | 1 (0, 1) | 0.0621 | |
| Adults in house | Mean (SD) | 2.06 (0.73) | 1.96 (0.68) | 2.01 (0.70) | |
| Median (Q1, Q3) | 2 (2, 2) | 2 (2, 2) | 2 (2, 2) | 0.5014 | |
| Number of adults smoking | Mean (SD) | 0.38 (0.74) | 0.23 (0.47) | 0.30 (0.61) | |
| Median (Q1, Q3) | 0 (0, 0) | 0 (0, 0) | 0 (0, 0) | 0.5328 | |
N/A, not applicable; SD, standard deviation.
Parents/carers reported that most patients did not receive antibiotic treatment in the four weeks prior to surgery (77%). There was a significant association between the number of infections in the past year and antibiotic use in the past month (Fishers exact test, P<0.001); a greater proportion of children who received antibiotics experienced a larger number of infections (more than 6) in the past year (71%), compared to those not given antibiotics (17%).
OM-6 survey results
In total, 70 of the 101 participants (69%) completed the follow-up survey for QoL measures. This included 36 parent/carers of the original 54 Aboriginal children (67%) and 34 of the 47 parent/carers of non-Aboriginal children (72%); Chi-squared testing indicated there was no significant difference in follow-up between Aboriginal and non-Aboriginal patients (P=0.5375). The proportion of Aboriginal to non-Aboriginal children in the follow-up population was 51% compared to 49%, respectively. Participants who were not followed-up were all unable to be contacted by phone (31%). The results for the OM-6 survey are shown in Table 2; for all children in the study, each domain, as well as overall QoL, was significantly improved after surgery (P<0.0001).
Table 2
| Outcome | ICC | Population | Baseline | Aboriginal effect | Time effect | Overall | |||
|---|---|---|---|---|---|---|---|---|---|
| 6 weeks post | Difference (95% CI) | P value | Type III | ||||||
| Physical suffering (OM6a) | 0 | All participants | 3.33 (3.00, 3.66) | 1.64 (1.34, 1.94) | −1.75 (−2.16, −1.34) | <0.0001 | |||
| Non-Aboriginal | 3.43 (2.98, 3.87) | 1.59 (1.07, 2.11) | −1.83 (−2.43, −1.24) | <0.0001 | 0.7080 | ||||
| Aboriginal | 3.24 (2.83, 3.66) | 1.56 (1.06, 2.07) | −1.68 (−2.25, −1.10) | <0.0001 | |||||
| Difference (95%) | −0.18 (−0.79, 0.42) | −0.03 (−0.75, 0.69) | |||||||
| P value | 0.5471 | 0.9375 | |||||||
| Hearing loss (OM6b) | 0 | All participants | 4.98 (4.68, 5.28) | 2.21 (1.80, 2.63) | −2.83 (−3.21, −2.45) | <0.0001 | |||
| Non-Aboriginal | 5.23 (4.76, 5.71) | 1.94 (1.41, 2.47) | −3.29 (−3.83, −2.76) | <0.0001 | 0.0193 | ||||
| Aboriginal | 4.76 (4.32, 5.20) | 2.35 (1.84, 2.87) | −2.41 (−2.92, −1.90) | <0.0001 | |||||
| Difference (95%) | −0.47 (−1.12, 0.17) | 0.41 (−0.33, 1.15) | |||||||
| P value | 0.1463 | 0.2726 | |||||||
| Speech impairment (OM6c) | 0.223 | All participants | 4.23 (3.85, 4.60) | 2.20 (1.79, 2.61) | −1.99 (−2.39, −1.59) | <0.0001 | |||
| Non-Aboriginal | 4.30 (3.77, 4.83) | 1.92 (1.32, 2.52) | −2.38 (−2.95, −1.81) | <0.0001 | 0.0614 | ||||
| Aboriginal | 4.17 (3.67, 4.66) | 2.54 (1.97, 3.12) | −1.62 (−2.17, −1.07) | <0.0001 | |||||
| Difference (95%) | −0.13 (−0.86, 0.59) | 0.62 (−0.21, 1.45) | |||||||
| P value | 0.7196 | 0.1383 | |||||||
| Emotional distress (OM6d) | 0.117 | 3.93 (3.57, 4.29) | 2.12 (1.75, 2.49) | −1.85 (−2.26, −1.45) | −1.85 (-2.26, −1.45) | <0.0001 | |||
| Non-Aboriginal | 3.68 (3.18, 4.19) | 2.21 (1.65, 2.77) | −1.48 (−2.05, −0.90) | <0.0001 | 0.0724 | ||||
| Aboriginal | 4.10 (3.64, 4.57) | 1.90 (1.35, 2.45) | −2.20 (−2.76, −1.65) | <0.0001 | |||||
| Difference (95%) | 0.42 (−0.26, 1.10) | 0.31 (−1.09, 0.48) | |||||||
| P value | 0.2233 | 0.4359 | |||||||
| Activity limitations (OM6e) | 0.155 | All participants | 3.09 (2.73, 3.45) | 1.97 (1.59, 2.36) | −1.16 (−1.63, −0.69) | <0.0001 | |||
| Non-Aboriginal | 3.06 (2.55, 3.57) | 1.76 (1.16, 2.36) | −1.30 (−1.98, −0.61) | 0.0003 | 0.5790 | ||||
| Aboriginal | 3.11 (2.64, 3.59) | 2.08 (1.50, 2.65) | −1.03 (−1.68, −0.39) | 0.0021 | |||||
| Difference (95%) | 0.05 (−0.65, 0.75) | 0.31 (−0.52, 1.14) | |||||||
| P value | 0.8849 | 0.4534 | |||||||
| Caregiver concerns (OM6f) | 0.079 | All participants | 4.02 (3.68, 4.36) | 2.31 (1.90, 2.72) | −1.79 (−2.21, −1.37) | <0.0001 | |||
| Non-Aboriginal | 4.00 (3.50, 4.50) | 2.30 (1.72, 2.89) | −1.70 (−2.31, −1.09) | <0.0001 | 0.6741 | ||||
| Aboriginal | 4.06 (3.59, 4.54) | 2.19 (1.62, 2.75) | −1.88 (−2.47, −1.29) | <0.0001 | |||||
| Difference (95%) | 0.06 (−0.63, 0.75) | −0.12 (−0.93, 0.69) | |||||||
| P value | 0.8604 | 0.7722 | |||||||
| Overall QoL (OM-6) | 0 | All participants | 3.94 (3.68, 4.19) | 2.07 (1.79, 2.35) | −1.93 (−2.20, −1.66) | <0.0001 | |||
| Non-Aboriginal | 3.97 (3.60, 4.34) | 1.92 (1.51, 2.33) | −2.05 (−2.44, −1.66) | <0.0001 | 0.4215 | ||||
| Aboriginal | 3.91 (3.56, 4.25) | 2.08 (1.68, 2.48) | −1.83 (−2.20, −1.45) | <0.0001 | |||||
| Difference (95%) | −0.06 (−0.56, 0.44) | 0.16 (−0.41, 0.73) | |||||||
| P value | 0.8102 | 0.5813 | |||||||
Difference = difference between aboriginal and non-aboriginal QoL estimates at each time point. ICC, intraclass correlation coefficient; QoL, quality of life; 95% CI, 95% confidence interval.
The OM-6 scores changed significantly after VT surgery across all domains for both Aboriginal and non-Aboriginal children. Although there was no significant difference between the groups at baseline for QoL domains, non-Aboriginal children showed higher hearing loss scores at baseline but recorded lower hearing loss scores at 6 weeks (5.23 down to 1.94) than Aboriginal children (4.76 down to 2.35), indicating significantly greater improvement in QoL in regard to the impact of hearing loss than was reported for Aboriginal children (P=0.0193). However, the change in overall QoL over time was not significantly different between Aboriginal and non-Aboriginal children.
Mixed modelling results for individual QoL domains and overall summary score over time by Aboriginal identification are also shown; higher model estimates were indicative of worse QoL while negative values for differences in estimates corresponded to QoL improvement.
Discussion
The QoL study presented an opportunity to investigate the impact of OM among Aboriginal and non-Aboriginal children residing in the HNELHD of NSW. Acknowledging the limitations of a small sized study, we think the geographical reach of approximately 400 km, from coastal Awabakal and Worimi country up to the north-western Gomeroi tablelands, provided a study cohort broadly representative of HNELHD children presenting with OM at public hospital ENT services. In this study, 53% of the VT surgery patients identified as Aboriginal, this is in a health service whose Aboriginal clientele comprises approximately 5% of the population.
Higher prevalence of Aboriginal children’s OM
Understanding the difference between the numbers of Aboriginal and non-Aboriginal children requiring specialist ENT surgery emerged as an area for further research. The QoL data do not provide an explanation for the higher numbers of Aboriginal children requiring VT tubes for treatment of OM. A similar pattern was observed in our earlier studies of the pathology of OME in the HNELHD (9). Our previous investigations found there were no differences between bacterial flora identified in middle ear effusion obtained from Aboriginal or non-Aboriginal children with OM. The findings from the earlier pathology investigations could not explain the higher prevalence of Aboriginal children that require ENT intervention (9).
Although their greater disadvantage in ear health is widely known, particularly in remote communities, there is a lack of research on health inequity of Aboriginal children living in urban areas. This is acknowledged by Bowes and Grace in their 2014 report for the ‘Closing the Gap Clearinghouse’ (10). In our QoL study: 58% of Aboriginal children receiving VTs lived in a major city area, compared with 70% of non-Aboriginal children; the remaining children lived in regional areas, reinforcing the fact that Aboriginal children’s OM has a wide geographical reach. While hearing loss has been correlated with education outcomes and incarceration rates, it is now considered by the Australian Medical Association to be a significant contributor to many more emotional, behavioural, social dysfunction and health issues that are over-represented in Aboriginal communities (2).
Study participants
We experienced a high level of uptake of the QoL study from both Aboriginal and non-Aboriginal families. Employing the OM-6 questionnaire to assess QoL in Aboriginal and non-Aboriginal children demonstrates the cross-cultural application of this survey and its potential as a research tool in our local health district. English language fluency was not a concerning factor in our NSW cohort, given English is the first language for most Australians born in NSW and only a very small percentage of study participants claimed non-Australian heritage (<1%). This interesting observation raises the importance of health literacy and the ability to understand the pathways to access health. Despite literacy being competent for participation in this study, the overall understanding in health literacy skills of the study participants indicates this could be an important factor for Aboriginal Australians’ ability to access ENT health care successfully in the public health system. This raises the possibility that families experiencing greater levels of social disadvantage, such as lower literacy levels, might not be as successful in navigating health pathways to ENT specialist care, a topic that warrants further investigation. Indigenous literacy levels are reported to remain low across urban, rural and remote regions; continued improvement in Indigenous literacy levels is a current Closing the Gap target (11).
The data comparing Aboriginal with non-Aboriginal participants showed that many similar characteristics emerged for a range of demographic factors relevant to ear disease: age at surgery, infection patterns, antibiotic use and living conditions. These findings differ from common patterns of socioeconomic differences reported for studies of Aboriginal ear disease in many remote Australian communities; marked disparities in living conditions are correlated with Aboriginal children’s higher rates of ear disease (12,13). This supports consideration of the social and geographical contexts when investigating the aetiology of ear disease in Aboriginal populations. The higher proportion of male to female Aboriginal and non-Aboriginal patients requiring ENT surgical intervention reinforced a pattern of male predominance reported previously for OME (1,14).
Limitations
The study is small in size and, although the entire cohort underwent VT surgery, there were differences in medical histories, which were not available for documentation. All recruitment was conducted by the research co-ordinator, resulting in a strong 100% response rate at the initial in-person meeting but a lower rate (69%) when participants were contacted by phone for the follow-up survey.
QoL
The improvement in OM-6 scores showed that parents/carers found specialist ENT surgical intervention resulted in an improvement in QoL for Aboriginal and non-Aboriginal children with recurrent or chronic ear disease, consistent with the findings of Chow et al., 2007 (7). The overall QoL score for this study was not dissimilar from the score for the Adelaide cohort. While we report a change in the mean OM-6 from 3.94 down to 2.07, Chow et al. reported a finding of 3.43 down to 2.07 following VT surgery (7). In both studies the changes in all domains and the change in total OM-6 scores achieved significance. Although the similarity is interesting, it should be noted that the South Australian study excluded patients having other ENT surgery, while our study included all VT patients on the ENT operating lists, regardless of other concurrent surgery. Our aim was to test the acceptability of the use of the OM-6 survey to the Aboriginal and non-Aboriginal parents/caregivers in our health service region, as opposed to conducting a rigorous validation of the study tool.
Rosenfeld et al. also reported exclusion criteria, related to perforation, prior VT insertion, other OM pathology, developmental issues and parent/caregiver English language ability (3). In order to assess the validity of the tool to measure the efficacy of a surgical intervention our study would require more detailed knowledge of patient medical histories, which was not available to the research team. However, it was reassuring to demonstrate that, within our health service population, the study tool was well accepted by parents and caregivers.
Health service access
Data for health service delivery were not collected during this project, but many parents/caregivers volunteered information to the study co-ordinator that very long waiting list periods had been a challenging feature of the pathway to specialist ENT surgical intervention. It is also possible that the high proportion of Aboriginal patients on the operating lists could, to some extent, reflect the benefit of a specific health pathway for Aboriginal children’s access to ENT care. Hunter New England Health Service has a co-operative partnership with the Aboriginal Community Controlled Health sector that creates a pathway for expedited care through the Aboriginal medical services provided with outreach by the members of the ENT department at John Hunter Hospital, Newcastle. However, many Aboriginal families access health care through mainstream GP practices (15).
Conclusions
Our study showed that the OM-6 questionnaire can be used effectively with Aboriginal and non-Aboriginal families in the HNELHD of NSW to investigate the impact of OM on children. The findings provide evidence that surgical intervention has a strongly positive effect on child QoL. The demographic characteristics suggest that families who access ENT specialist care successfully through the public health system demonstrate many similarities in their living circumstances. The results do not explain the difference in prevalence of OM between Aboriginal and non-Aboriginal children, indicating there is a need for more research on Aboriginal children’s ear disease in NSW if the gap in ear and hearing health is to be closed.
Acknowledgments
The Newcastle ear research team gratefully acknowledges longstanding research relationships in the study of otitis media quality of life with staff and community members of the Tamworth Aboriginal Medical Service, Tobwabba Aboriginal Medical Service (Forster) and Armajun Aboriginal Health Service (Inverell). We are also very thankful to the staff of the operating theatres and paediatric wards at John Hunter Hospital, Newcastle, and the Maitland Hospital for accommodating the quality of life research activities in their workplaces.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at https://ajo.amegroups.com/article/view/10.21037/ajo-21-24/rc
Data Sharing Statement: Available at https://ajo.amegroups.com/article/view/10.21037/ajo-21-24/dss
Peer Review File: Available at https://ajo.amegroups.com/article/view/10.21037/ajo-21-24/prf
Funding: This study was supported by competitive grant funding awarded by the
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://ajo.amegroups.com/article/view/10.21037/ajo-21-24/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). Ethics approval for the Quality of Life project was obtained from the Hunter New England Human Research Ethics Committee (ref: 2020/ETH00170). The use of data collected using the OM-6 survey tool among HNELHD Aboriginal research participants was approved by the Aboriginal Health and Medical Research Council Ethics Committee (1703/20). Informed consent for participation in the OM-6 study was obtained by the research co-ordinator from all parents/caregivers prior to their child’s surgery and it was explained that all medical procedures were independent of the research study.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Kong K, Coates HL. Natural history, definitions, risk factors and burden of otitis media. Med J Aust 2009;191:S39-43. [Crossref] [PubMed]
- 2017 AMA Report card on Indigenous health—a national strategic approach to ending chronic otitis media and its lifelong impacts in Indigenous communities. Available online: https://www.ama.com.au/article/2017-ama-report-card-indigenous-health-national-strategic-approach-ending-chronic-otitis (accessed May 2021).
- Rosenfeld RM, Goldsmith AJ, Tetlus L, et al. Quality of life for children with otitis media. Arch Otolaryngol Head Neck Surg 1997;123:1049-54. [Crossref] [PubMed]
- Homøe P, Heidemann CH, Damoiseaux RA, et al. Panel 5: Impact of otitis media on quality of life and development. Int J Pediatr Otorhinolaryngol 2020;130:109837. [Crossref] [PubMed]
- Kubba H, Swan IR, Gatehouse S. How appropriate is the OM6 as a discriminative instrument in children with otitis media? Arch Otolaryngol Head Neck Surg 2004;130:705-9. [Crossref] [PubMed]
- Heidemann CH, Godballe C, Kjeldsen AD, et al. The Otitis Media-6 questionnaire: psychometric properties with emphasis on factor structure and interpretability. Health Qual Life Outcomes 2013;11:201. [Crossref] [PubMed]
- Chow Y, Wabnitz DA, Ling J. Quality of life outcomes after ventilating tube insertion for otitis media in an Australian population. Int J Pediatr Otorhinolaryngol 2007;71:1543-7. [Crossref] [PubMed]
- NSW Health, Hunter New England Health. Available online: https://www.hnehealth.nsw.gov.au/our_services2/aboriginal-health (accessed 31.01.21).
- Ashhurst-Smith C, Hall ST, Walker P, et al. Isolation of Alloiococcus otitidis from Indigenous and non-Indigenous Australian children with chronic otitis media with effusion. FEMS Immunol Med Microbiol 2007;51:163-70. [Crossref] [PubMed]
- Bowes J & Grace R 2014. Review of early childhood parenting, education and health intervention programs for Indigenous children and families in Australia. Issues paper no. 8. Produced for the Closing the Gap Clearinghouse. Canberra: Australian Institute of Health and Welfare & Melbourne: Australian Institute of Family Studies.
- Commonwealth of Australia, Department of the Prime Minister and Cabinet, Closing the Gap Prime Minister’s Report 2017.
- Morris PS, Leach AJ, Silberberg P, et al. Otitis media in young Aboriginal children from remote communities in Northern and Central Australia: a cross-sectional survey. BMC Pediatr 2005;5:27. [Crossref] [PubMed]
- Lehmann D, Arumugaswamy A, Elsbury D, et al. The Kalgoorlie Otitis Media Research Project: rationale, methods, population characteristics and ethical considerations. Paediatr Perinat Epidemiol 2008;22:60-71. [Crossref] [PubMed]
- Zernotti ME, Pawankar R, Ansotegui I, et al. Otitis media with effusion and atopy: is there a causal relationship? World Allergy Organ J 2017;10:37. [Crossref] [PubMed]
- Australian Institute of Health and Welfare 2016. Australia’s health 2016. Australia’s health series no. 15. Cat. no. AUS 199. Canberra: AIHW.
Cite this article as: Kong KM, Hall ST, Palazzi K, Faulkner J, Hall B, Eisenberg R, Jefferson N, Cope D, Huang J, Corlette T, Young N, Blackwell CC. Otitis media and quality of life in NSW Aboriginal children. Aust J Otolaryngol 2022;5:5.


